South Africa learns from HIV/Aids crisis on working with charities
Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
On a sunny weekday morning in Alexandra, a crowded Johannesburg township where Nelson Mandela lived as a young man, 49 children crowd around a teacher as she leads them through a song in Xitsonga, one of several languages spoken in the neighbourhood.
Each day, the group of three- to six-year-olds at this early childcare centre receive a hot breakfast and lunch, something they are not always guaranteed at home, says Nyiko Mabasa, a 37-year-old teacher at the centre run by Save the Children South Africa.
Ms Mabasa lives in Alex, as it is known, and regularly visits her students’ homes to watch, among other things, for signs they are malnourished. She refers them to a doctor if they are.
That is a crucial service in South Africa, where about a quarter of children under age three suffer from stunting, a problem that can stem from poor nutrition and affects everything from how well they do in school to their later employment opportunities. In Alex and at nearly 200 other early childcare centres in the country, Save the Children is working to improve nutrition.
“We’re a middle-income country,” says Sue Jones, health and nutrition programme manager for Save the Children South Africa. “It should be a lot better.”
South Africa spends an average of $570 per person on health a year, more than any other country in southern Africa, according to World Bank data. This is due in part to the country’s extensive HIV and tuberculosis programmes. Compared with some of its neighbours, the healthcare system works well, particularly in bigger cities, and the government has comprehensive healthcare policies in place at a national level, observers say.
But there remain significant gaps in access to high quality healthcare on the ground. Only a fraction of the population can afford private healthcare. The many who rely on the public system have difficulty getting the help they need due to lack of staff and equipment at their local clinics, or inability to reach specialist care at hospitals that may be far away.
For years, not-for-profit, charitable and other grassroots organisations in South Africa have helped fill those gaps. Unlike other countries in Africa, where charities stand in directly to provide essential healthcare, organisations in South Africa often work in tandem with the government to meet public health goals or help connect vulnerable patients to the public healthcare system.
“South Africa has the best policies,” says Sanjana Bhardwaj, chief of health, nutrition and HIV/Aids for Unicef in South Africa. “The struggle here is making those policies work on the ground.”
In some cases, independent organisations have been instrumental in helping develop those policies. In the late 1990s, as the gravity of the HIV crisis in South Africa came into focus, a coalition of charities worked together to demonstrate the desperate need for affordable anti-retroviral drugs, despite the then government’s infamous denial of Aids. Médecins Sans Frontières, along with South Africa-based Treatment Action Campaign and other local partners, helped quietly bring generic anti-HIV drugs into the country and treated patients at a government clinic in a Cape Town township where infection rates were soaring.
After that coalition demonstrated affordable, life-saving HIV treatment was possible, and lobbied for several years, the government changed its policies. It now runs the largest HIV drug treatment programme in the world.
“Although the overarching system is functional, there are lots of gaps,” says Amir Shroufi, MSF’s medical co-ordinator in South Africa. “By addressing those gaps, our aim is not just to benefit a relatively small number of people but to demonstrate strategies that can be broadly replicated in the country.”
The success of overcoming the HIV epidemic holds an important lesson for the government, experts say. Battling HIV was a success because “everyone came to the party,” says Mosa Moshabela, head of the department of rural health at the University of KwaZulu-Natal. “If we got everyone to come to the party for all the other problems we have, we are much more likely to win than trying to tackle it on our own.”
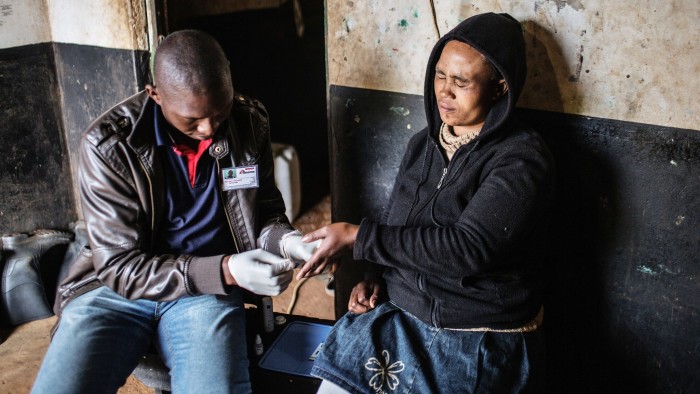
That is particularly true when it comes to supporting the tens of thousands of community health workers employed by non-governmental organisations across the country. They provide a critical service by visiting patients at home, both in crowded urban neighbourhoods like Alexandra and remote rural areas, and linking them with government services.
Mr Moshabela thinks the government should formally recognise more of those workers as healthcare professionals. “They are responding to unmet needs in the community,” he says. “Why are we not legitimising them?”
In Alex, Ms Mabasa considers it part of her job to make sure parents have as much information as possible about keeping their kids healthy. It is not only malnutrition she is monitoring. Sitting at a desk in the brightly painted centre while the students play outside, Ms Mabasa points to a stack of consent forms that she has reminded parents to sign. The provincial government runs an emergency immunisation campaign following a recent measles outbreak, and government healthcare workers are due any day to visit the centre to carry out vaccinations.
“I tell the parents why it’s important to immunise their kinds. Some parents take it seriously, and some don’t,” Ms Mabasa says. But she keeps trying. “When a child gets sick, it’s so painful for me.”

Comments