Pioneering surgery on the plains of Western China

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
Thousands of kilometres from the cities of China’s eastern seaboard, millions of Tibetans, Kazakhs, Mongols and other ethnic groups live as nomadic herders on vast grassy uplands in the country’s western reaches, dependent on yak, cows and sheep for milk and meat through sub-zero winters.
These regions, with their natural beauty and cultural diversity, are also home to rare tapeworms less than 3mm long, which spread from wild rodents to livestock and, through contact with dogs, to humans. They cause cysts that slowly enlarge in people’s internal organs. Though symptoms can go unnoticed for years, the result of infection with the disease, echinococcosis, is generally years of suffering followed by a premature death.
A sip of water polluted with parasites from dog faeces in a river near his home in the countryside of China’s Xinjiang region was probably all it took for Tang Zhu, 32, to contract the disease. It went undetected for years before spreading from his liver to his brain, causing him to go blind, suffer seizures and have difficulty walking.
Xinjiang, a vast region abutting central Asia, is home to snow-capped mountains, deserts and, more recently, the world’s biggest screening and prevention programme for echinococcosis. As he was born locally, Tang qualified for diagnosis and care at what has become a leading surgical centre, Xinjiang Medical University’s affiliated hospital in the regional capital of Urumqi.
Tang was prescribed albendazole to combat the disease and underwent years of chemotherapy to treat cysts in his lungs and liver. Wen Hao, one of the hospital’s surgeons, recalls thinking it would be “impossible” to treat Tang. But, against expectations, Tang survived and found work as a masseur in a hospital. “Without treatment, 10 years ago he would have died,” Wen says.
Deadly varieties of echinococcosis have claimed lives for centuries in rural areas all over the world, from Iran to France, Kenya and the US, with around a million patients globally and tens of thousands of deaths caused each year. Of the 200,000 new cases estimated to emerge annually, more than half occur in China, but it is only since the late 1990s — thanks to international research revealing the scope of the disease, and political will to spend on areas left behind during China’s economic growth — that authorities have made significant progress on treatment and prevention.
There are two main varieties of echinococcosis, depending on the genus of parasite causing the infection. The most common, cystic form (known as CE) is caused by parasite embryos lodged in organs — generally the liver but also the lungs and, more rarely, the brain — where they develop into larvae in the form of fluid-filled cysts.
In his office at the hospital, surgeon Sailike Duishanbai brandishes a jar containing a transparent sphere resembling a jellyfish, extracted from a brain of a patient with CE. An ethnic Kazakh, Duishanbai grew up in a herding family and knows the disease’s dangers. “It is very common in nomadic ethnic groups,” he says. “It’s very expensive to treat.”

Tang has alveolar echinococcosis (AE), a rarer but more dangerous form of the disease with a mortality rate of more than 90 per cent. It is more dangerous in part because it has a longer incubation period, from five to 15 years, meaning patients may only be diagnosed decades after contracting it. More than 90 per cent of the world’s AE cases are thought to occur in China, resulting from rodents with the tapeworms that are found largely in this part of the world.
“Alveolar is more difficult [to operate on] than cancer — it’s ‘more stuck’ to vital structures in the brain,” Duishanbai explains. One of the few members of his community to attend university, he now carries out cyst-removal operations, which can last for more than 11 hours. But he relishes the work he describes as “very adventurous, risky”.
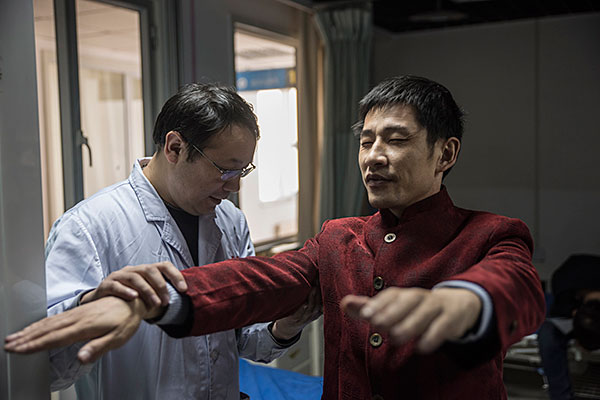
Tang sits on a hospital bed while Duishanbai tests his reflexes. A crowd of onlookers gathers — the facility draws patients from across Xinjiang and its corridors are filled with women in bright headscarves and men wearing the square doppa hats that are common among the region’s Uighur ethnic group. The Uighurs are mostly Muslims with stronger historical links to central Asia than China.
Xinjiang tends to hit global headlines following periodic clashes between security forces and the 10-million-strong Uighur population in which hundreds of people on both sides have been killed in recent years. As a result, security in Urumqi is tight, with mandatory checks on people and bags around public buildings. A few days ago, an “anti-terror” demonstration has taken place in the city involving 10,000 armed police.
None of that deters Wen Hao as he blithely waves his way past a guard clad in black and brandishing a shield and baton at the hospital’s entrance. He darts into a ward and places his hand on the shoulder of a 26-year-old CE patient who has recently received the hospital’s most advanced treatment, which Wen refers to ominously as “radical resectioning” — removing the liver whole and stripping it of cysts before replacing it.
“Five years ago if there was a lesion like this, surgeons could do nothing. He would have died after one or two years,” Wen says, beaming. “It’s the only place in China with this technology.” The patient’s mother is at her son’s bedside and bursts into tears: “He’s better now,” she sobs. “Thanks so much.”
Wen’s office is in a building built by the Soviet Union in the 1950s, when China’s recently victorious Communist party began moving members of the ethnic Han majority to Xinjiang in large numbers to secure the region. Doctors encountering the disease there made early efforts to treat it, but operations were crude, with surgeons sometimes puncturing cysts inside patient’s organs, unleashing floods of parasitic larvae.

The story of China’s modern treatment programme for echinococcosis follows an unlikely path to Xinjiang from north-west England. Wen Hao was a PhD student with Dr Philip Craig at Liverpool School of Tropical Medicine and later the University of Salford. Craig has had a celebrated career as a parasitologist, once even ingesting a tapeworm for an experiment (he wrote soberly in a paper that “abdominal discomfort [peaked at] around 15-19 weeks post-infection”). In the 1980s, he was one of the first foreign researchers to chart the disease in China. “We realised there was a big problem,” he says.
Soon, scientists from several countries, including France and Japan, were being funded by international bodies, including the European Commission and the US National Institutes of Health, to measure the burden of the disease in China. A trip in the 1990s to a remote part of Gansu province revealed conditions resembling “the middle ages in Europe”, says Dominique Vuitton of the University of Franche-Comté in eastern France. “It was the most neglected of neglected diseases . . . the burden was really not known,” she says. “Just the tip of the iceberg arose in the hospitals.”
Early infection figures shocked researchers, with rates of more than 10 per cent of the population in some counties. The researchers took their findings to central government officials in Beijing, eliciting government support starting in the early 2000s with funding for treatment with the drug albendazole, which was developed in the 1970s and can slow the growth of cysts.
Funding for operations also increased — to Rmb8,000 (about $1,100 in today’s terms) per patient nationwide, plus variable contributions from local government insurance schemes. Mass screening — through methods such as ultrasound scans that reveal cysts — showed how big a burden it could become on the Chinese healthcare system, Vuitton says. In the early 2000s, when China was being criticised for neglecting its western provinces, it was a way for central government to demonstrate it did actually care, she adds.
The cystic form of the disease was also present in the south of France, where Wen Hao was the first of several Chinese doctors to train with Vuitton’s team. He returned in the 1990s with a fondness for red wine and mastery of the latest surgical techniques. Just 20 years later, the team he leads in Urumqi is acknowledged to be the most advanced in the world.
In the past decade, China has rolled out the largest prevention programme ever created for the disease, including drug treatment for millions of dogs and vaccination for livestock. To test the results of the programme, thousands of canine stool samples are analysed each year in Urumqi. “They keep the dog faeces here,” researcher Zhang Wenbao says, pointing to a tall stainless steel freezer in the hospital’s lab. “They are frozen for a week then tested.”
Zhang admits the commercial imperatives for further drug development are small. “How big is the market?” he asks. “The market is poor people. We asked companies for investment and no one [was] interested. The big problem is investment.”
Severe though the situation in Xinjiang might be, the heaviest burden of the disease is found on the Tibetan plateau. Both main varieties of echinococcosis are found in the region, spread by the Tibetans’ use of dogs to protect their yaks, large numbers of strays and lack of awareness about sanitation.
“Getting up to the Tibetan plateau for the first time, it was pretty staggering — even more horrific for public health than what I’d seen in Africa,” says Craig. Beijing has funded treatment and dog drug schemes and, while progress has been made, he adds: “I don’t think the control programme and the national programme are reaching Tibetan counties very well.”

The hospital in Urumqi now sees dozens of Tibetan patients a year, including several Buddhist lamas. Aga, a Tibetan herder, was diagnosed seven years ago, but local hospitals were unable to remove his cysts. He says that the dog drug programmes have yet to reach his county in western Sichuan province’s remote Nagchu prefecture.
Looking at a scan of Aga’s torso is Shao Yingmei, a doctor who thinks nothing of downing six cans of energy drink during a 20-hour cyst-removal operation. Speaking in Mandarin, she reminds Aga of prevention methods such as not feeding dogs raw meat and the importance of hand-washing, as Aga stares uncomprehendingly. “We try and find translators,” she says, but the hospital has no Tibetan-language materials to distribute.
Aga’s trip was partly funded by government insurance and subsidies, but most will need to pay surgery fees equivalent to tens of thousands of yuan out of their pocket — a fortune for herders whose monthly income is likely to be in the hundreds. Stephanie Hua, a Tibetan charity worker who focuses on the disease, says that in most cases, patients are asked to pay half of their medical fees. “If there is no help from the government it can bankrupt a family,” says Hou Yanyan of the Xinjiang centre for disease control. “There can be situations where the disease drives people into poverty.”
The payment situation remains politically sensitive. When one patient’s wife begins to complain about lack of support, a doctor cuts her off. “Don’t listen!” he says, shepherding reporters away.
In a mainly Tibetan region of Qinghai province in central China, locals say the dog drug programmes have been hampered by corruption, where funds allocated to the medication have been misappropriated. Sitting in his spartan concrete house close to the shores of Qinghai Lake, country doctor Ma Youqing raises his shirt to reveal a scar from an operation. “I too got the disease,” he says. Afterwards, pacing towards his herd of sheep and cows chewing on the stiff grass, he says he sold nearly half his animals to pay for the operation.
Public health researchers say the prospects of the disease disappearing from the Tibetan plateau are slim, given its vast size. “All the successful elimination programmes have been island programmes,” says Craig, citing New Zealand, Tasmania and Iceland as examples. “What’s on the cards perhaps is county-level elimination. Until there is a [human] vaccine, transmission will still go on.”
Lhamo Dolma, 39, who lives a short drive away, says she was diagnosed with the disease three years ago but had had the illness for years. To pay for operations, one of which was to remove a red cyst she describes as “like an apple” from her stomach, she sold her entire flock of more than 100 sheep and is dependent on relatives. “You cannot work — you are too tired. I just stay in the house,” she says. “It’s a very bad disease”.


Comments