FT People of the Year: BioNTech’s Ugur Sahin and Ozlem Tureci

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
In the 11 months since they devoted themselves to stemming the deadliest pandemic in over a century, Ozlem Tureci and Ugur Sahin’s precious few private moments have been spent exercising along deserted suburban streets near their home in the German city of Mainz, listening to ’80s pop playlists.
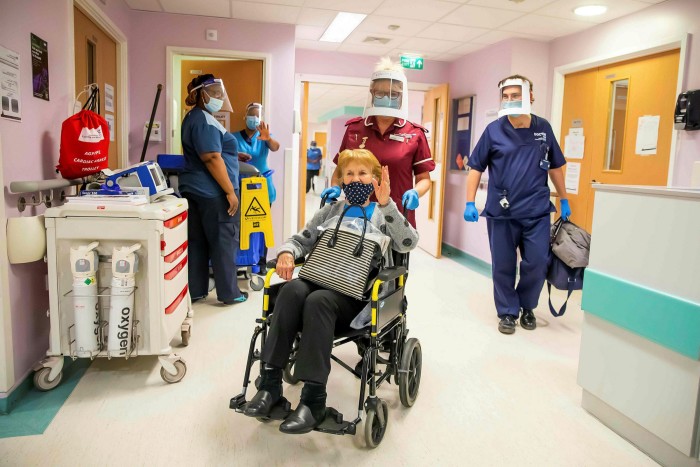
Deluged by paperwork from regulators around the world last week, the co-founders of BioNTech missed the TV footage of 90-year-old Margaret Keenan rolling up her sleeve at a hospital in Coventry in the UK to become the first patient injected with their approved Covid-19 vaccine — the news trickling in via messages from friends and colleagues.
The symbolism of those images, however, was unmistakable: it effectively kickstarted humanity’s fightback against a disease which has claimed more than 1.6m lives.
“We were nervous,” admits Dr Sahin, whose quiet confidence has seemed shatterproof over the past year. Despite having seen their jab administered to more than 22,000 people in clinical studies across six countries, he says “it is different when people are vaccinated for the first time outside a trial, in the real world setting”.
The mere fact that a safe and effective inoculation is available less than a year after the genetic sequence for a new, pneumonia-like pathogen was released puts the achievement by Dr Sahin and Dr Tureci, who are the FT’s People of the Year for 2020, alongside the greatest medical breakthroughs of our time.
Science is by its nature a slow, painstaking business. Hypotheses have to be challenged and new ideas tested to exhaustion. Failure is an essential part of the process.
Roughly six out of 10 vaccine candidates are never approved, even when carefully chosen over several years, and without having to contend with a backdrop of healthcare systems being brought to their breaking point or a stricken global economy.
All of which makes the speed at which the married couple managed to produce a jab that is more than 95 per cent successful in preventing disease even more remarkable.
The multibillion-euro effort the two doctor-scientists launched, codenamed Project Lightspeed, led to “the fastest development of a vaccine since Edward Jenner inoculated his gardener’s son with cowpox in 1796,” says Paul Hunter, professor of medicine at University of East Anglia. The previous modern record for a vaccine, achieved in the 1960s for mumps, was four years.
BioNTech, whose vaccine uses a revolutionary new technology that could be used in treating cancer, is not alone. Moderna, the US biotechnology company, is close to getting approval for a vaccine that is almost equal in its effectiveness to the product developed by their German colleagues. Oxford university and AstraZeneca’s vaccine might have a similar response rate at some doses — and given its lower manufacturing costs, could be widely used in the developing world. Chinese and Russian vaccines might turn out to be highly effective once they undergo further overseas tests.
As creators of the first vaccine to win approval by two of the world’s most credible regulators, however, the FT’s award has gone to Dr Sahin and Dr Tureci. They are the symbol of a remarkable scientific and business success story.
Even a few months ago, scientists suggested it would be a major achievement to get a vaccine so quickly that was 70 per cent effective: instead, there are at least three that could be 90 per cent plus. Taken together, they represent a triumph of innovation.
“If you had predicted in January when Covid-19 first appeared that you’d have an effective vaccine approved less than a year later, people would have laughed in your face,” says Michael Head, senior research fellow in global health at Southampton university.
Relief and vindication
Sitting around the breakfast table in January with Dr Tureci — his research partner and wife — the 55-year-old Dr Sahin discussed a report in the Lancet medical journal on a respiratory disease that had run riot through China’s Hubei province.
The evidence, he felt, pointed to an alarming rate of infection and the threat of a more rapid spread than even the study’s authors had grasped.
Two months before the World Health Organization had even declared a pandemic, Dr Sahin suggested that the 12-year-old firm devote the vast bulk of its meagre resources to coming up with a vaccine.
“He has a very high hit rate when it comes to predicting outcomes,” Dr Tureci says of her husband — a trait she jokingly admits was initially “annoying”. She and the rest of the company’s board approved the plan soon after.
For Dr Sahin and Dr Tureci — whose insistence that the technology they have helped develop could herald a medical revolution was once dismissed as “science fiction” — the successful coronavirus vaccine has provided as much vindication as relief.
The couple, who between them have authored hundreds of academic papers, filed hundreds of patents, founded two non-profit organisations and two billion-euro businesses, faced scepticism from much of the medical establishment right up until this year.

The groundwork that led to their breakthrough was laid over several decades, in which the two softly-spoken researchers were forced to move out of the comfort zone of their labs and to become entrepreneurs, educators and evangelists.
After meeting as trainee doctors on a blood cancer ward in south-west Germany in the early 1990s, the couple discovered that they shared similar backgrounds — both sets of parents had migrated from Turkey in search of economic opportunity. They also realised that their core interest was not in purely academic science, but in applied science.
“First and foremost, we are physicians,” says Dr Tureci, who ran the duo’s first company, Ganymed, and is chief medical officer at BioNTech.
Their lives’ work, which eventually centred on a vaccine platform so niche that just seven years ago only 150 people attended the first global conference dedicated to the technology, was always “about providing solutions for the patient”, she adds. “Science was a tool to achieve that. This was never about just understanding the mechanism because it is so beautiful.”
While still practising medicine, Dr Tureci and Dr Sahin, who confesses to being a little more driven by the “beauty of mathematics, science and biology” than his wife, became obsessed with tackling cancer. They started developing a tool to discover and use naturally occurring antigens that could prompt the body to fight tumours.
Their vision, however, suffered a blow in the mid 1990s. Cancers, it turned out, were too varied to be attacked by a catch-all drug.
“We learned from our studies that human cancers are highly diverse,” Dr Sahin recalls. “We understood that we needed a versatile technology to enable personalised vaccine approaches.”
What followed was a frenzied period in which the couple balanced their clinical duties with stolen moments in the lab testing a plethora of technologies that were found wanting — before they encountered an overlooked platform that they immediately believed could transform medicine.
Messenger RNA, first discovered in 1961, carries genetic information copied from DNA to create the proteins that build and control the body’s organs and tissues. If exploited correctly, the couple believed, mRNA could act as a traffic warden for the immune system, controlling, modulating and redirecting the body’s resources to fight specific cancers and pathogens.
Their conviction was not shared by many.
“I was among the first to tell [Sahin] it was crazy, that it's never going to work,” recalls Matthias Kromayer, a PhD in molecular biology and biochemistry who leads life science investments at Munich-based venture capital firm MIG, a backer of Ganymed and BioNTech.
His dismissal was not unreasonable. Unlike DNA, mRNA is extremely unstable, and is usually degraded by enzymes within minutes of fulfilling its function. Early experiments with mRNA “were very underwhelming”, says Dr Sahin.
Realising that mRNA vaccines would require years of research and optimisation before being fit for purpose, the couple forged ahead with the development of more established biological compounds, known as monoclonal antibodies, which they found to be highly effective against stomach, pancreatic and ovarian cancers.
In 2001, the couple founded Ganymed — a spin-off from the university, to develop therapeutic antibodies. Unlike many researchers who recoil at the transactional nature of the commercial world, they buried themselves in business studies, learning from online videos and a Business Plan for Dummies book that still sits on the shelf of Dr Sahin’s sparsely-furnished office, nestled among tomes on nucleic acids.
“They were not business people when they started out,” says Mr Kromayer, who had studied mRNA himself. “They are one of the very few examples of people who have transitioned from being scientists to also being business people.”
That mindset would pay off this year, when BioNTech’s team, shielded from the bureaucracy of larger multinationals, was able to develop 20 Covid-19 vaccine candidates in a matter of weeks, using a row of labs on the company’s start-up style campus, and forming rotas on a whiteboard in the corridor.
Decisions by the board on bonus pay and the division of responsibilities were taken quickly and Dr Sahin cycled in regularly to oversee the research.
“None of the speed, none of the innovation, none of the quick decisions, none of the risk-taking, none of the non-political thinking would have been possible in any of the large pharma corporations,” says Mr Kromayer.


mRNA mission
Despite the enormous success of Ganymed, which was sold for $1.4bn, in 2016, in Germany’s biggest biotech deal, the couple never gave up on mRNA. While running the business, they continued their research at Mainz university. Under a programme called “NT — Novel Technologies”, they filed dozens of patents which later formed the basis of BioNTech, whose eponymous capital letters are a tribute to that time. The couple even escaped to the lab to do some work on their wedding day.
By 2008, the Sahin and Tureci team’s first major accomplishment was to protect and optimise the vulnerable mRNA molecule, leading to an exponential increase in stability.
The advance was enough to convince MIG to invest in BioNTech, and to introduce the couple to billionaire twins Andreas and Thomas Strüngmann. After their initial meeting, Mr Strüngmann recalls, he had a “gut feeling that these are the people who will make [the promise of mRNA platforms] come true”, swayed as much by their personalities as their scientific presentations.
Realising that there would be a rush on talent once the advantages of mRNA platforms became clearer to mainstream science, Dr Sahin and Dr Tureci set about building a pipeline of their own, by investing in education.
Armed with a grant of €40m from the German government, they helped launch a cluster of excellence to attract young scientists, and set up a non-profit called TRON, for “translational oncology”, with their mentor, the immunologist Christoph Huber, which became a breeding ground for researchers who would later form the core of the BioNTech Covid-19 team.
At around the same time, they also met mRNA pioneer Katalin Kariko, a Hungarian-born scientist shunned by superiors at the University of Pennsylvania whose patented innovation was used as the basis for the successful Covid-19 vaccine.
Beyond a small group of venture capitalists, however, there remained few believers in the economic prospects of the trio of mRNA biotechs, which include Boston-based Moderna and local rival CureVac.
“One year ago, nobody knew BioNTech in Germany,” says the 70-year-old Mr Strüngmann, one of the country’s richest men. “Now they say we always knew BioNTech was a great company.”

The innovation cycle
Just three months after Dr Sahin’s Lancet revelation, BioNTech became the first private company in Europe to proceed to clinical trials of a Covid-19 vaccine, after successful results from tests in monkeys and mice.
All along, Dr Sahin, who maintained “the virus could be successfully tackled by a vaccine”, believed that with enough goodwill from regulators, a jab could be on the market by the end of the year.
Underpinning this belief was the key advantage of mRNA that had led the couple to relentlessly pursue the platform for decades — the ability to produce multiple versions of the molecule within days, rather than having to create cell cultures in a Petri dish as more conventional vaccines would do.
“We were forced when we started with this type of personalised cancer trials to develop testing and manufacturing processes which were very fast, very agile and very adaptable,” says Dr Tureci.
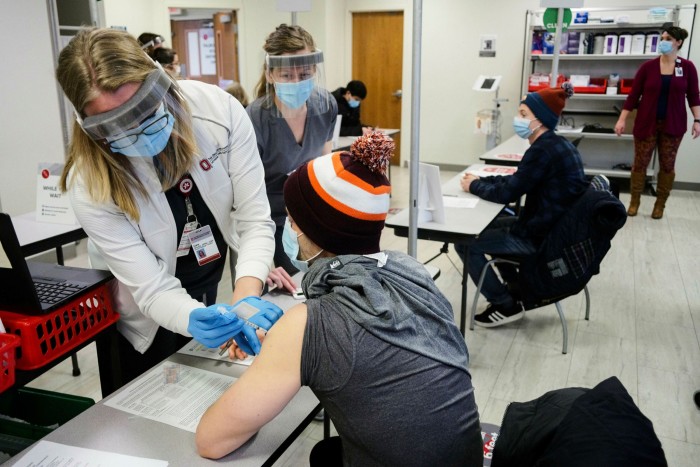
With the help of US partner Pfizer, and a German government grant that allowed BioNTech to expand its production facilities, hundreds of thousands of vials containing BNT162b2 started making their way to clinics in the UK, US, and Middle East earlier this month, in preparation for the largest mass vaccination campaign in history.
But the record-breaking development of the jab will probably have much broader repercussions.
“It is absolutely extraordinary that this new approach to vaccination — injecting chemical RNA into the muscle — has come through so quickly and proven to be so effective,” says Peter Openshaw, professor of medicine at Imperial College London. “It opens up a whole new field of vaccinology.”
The next coronavirus, Prof Openshaw suggests, could be tackled even faster, as drugmakers would “just need to reprogramme the chemical synthesis” of existing mRNA vaccines. Dozens of mRNA cancer therapies, immunisations for rare diseases and treatments for HIV and tuberculosis could also now be fast-tracked, as investment pours into the field.
Although the development of cancer drugs is a slower process, mRNA companies “will benefit from the huge safety database” accumulated in the Covid-19 large-scale trial, says Dr Sahin.
Young researchers will also be tempted to experiment with the molecule, says Prof Huber. “It was a DNA innovation cycle,” he says, “it is now an mRNA innovation cycle.”
Dr Tureci and Dr Sahin, both of whom still teach at the university hospital and at TRON, do not relish the attention they are now receiving, or the growing calls for them to be awarded a Nobel Prize.
Person of the Year
Browse profiles of all previous winners of the FT award:
2019 SATYA NADELLA The chief executive who presided over an era of stunning wealth creation
2018 GEORGE SOROS The standard bearer for liberal democracy, an idea under siege from populists
Every other winner From tech whistleblower Susan Fowler in 2017 to European Commission president Jean Rey, the first recipient of the award in 1970
Nor do they appreciate being used as a political prop — with sensationalist headlines hailing them as the ideal migration success story, rather than focusing on the merits of their research.
Last month, Armin Laschet, the premier of Germany’s most populous state and a potential successor to Angela Merkel, urged the hard-right Alternative for Germany party to “think about such people” when they talk about immigration.
Dr Tureci says she understands that the pair “tick a couple of boxes that people are interested in”. But she agrees with Dr Sahin, who says he would rather “talk about our science” than the pair’s background.
If there is a broader lesson for society from their success, the couple want it to reflect the motto of Dr Sahin’s school in Cologne, named after children’s author Erich Kästner. It reads: “Es gibt nichts Gutes, außer man tut es” — “Nothing good happens if one doesn't make it happen.”
More scientists, they say, need to venture into the worlds of business, technology and education, and marry their expertise with application.
Or as Dr Sahin puts it: “We always say you have to combine ‘explore’ with the right amount of ‘exploit’.”
The other vaccines

Moderna
Moderna is following swiftly in the footsteps of BioNTech and Pfizer, with its Covid-19 vaccine likely to receive US emergency approval by the end of the week.
The Boston-based biotech group is also a pioneer in mRNA technology, having worked to prove it can be a platform for both vaccines and therapeutics for over 10 years.
Moderna’s Covid-19 vaccine achieved an almost equivalent efficacy rate of 94.1 per cent in its phase 3 trial, and reported similar safety data. Perhaps the biggest practical difference between the vaccines is that Moderna’s can be stored at normal medical freezer temperatures, rather than the ultra cold ones required by the BioNTech/Pfizer vaccine.
The company has taken far more money from the US government — up to $4.1bn for development, including trials, and manufacturing. Last week, Operation Warp Speed, the government’s Covid vaccine programme, ordered another 100m doses by the second quarter of next year, bringing its total pre-order to 200m.
Oxford/AstraZeneca
Like Dr Tureci and Dr Sahin, Sarah Gilbert and her colleagues at Oxford university were quick out of the blocks when a mysterious new virus was identified in China.
Their vaccine, developed with AstraZeneca, is made from a weakened version of a common cold virus. It is reprogrammed to carry the genetic sequence of part of the coronavirus into human cells, where it stimulates the recipient’s immune system to repel the disease.
In November, they announced the vaccine has a 70 per cent efficacy rate — less than rivals BioNTech/Pfizer and Moderna. The additional claim that a different dosing regime had produced 90 per cent efficacy was met with confusion, particularly when it was learnt that the vaccine had yet to be tested in over-55s.
But, the vaccine retains two big advantages. AZ's decision to sell it at cost means it is a snip at around $3 a dose, and it can be kept at normal fridge temperatures. These qualities offer hope that it can protect millions in the developing world in the coming months.
Sinovac
CoronaVac, the Covid-19 vaccine developed by Beijing-based Sinovac Biotech, is the 21-year-old pharmaceutical group’s opportunity to secure a win for China’s ambitions to establish itself as a vaccine exporter.
Publicly released results of early stage clinical trials of the jab, which uses a chemically inactivated version of Sars-Cov-2 to spark an immune response, showed the vaccine to be safe and able to create virus neutralising antibodies in 98 per cent of cases.
But progress stalled as Sinovac had to seek partners overseas to carry out large-scale phase 3 efficacy trials, due to virus transmission being almost entirely halted in China. Trials are ongoing in Brazil, Indonesia, Turkey and Chile, but the company has yet to announce the vaccine’s effectiveness.
Despite the delay in concluding trials, Sinovac has already begun administering the vaccine to tens of thousands in China as part of a limited-use programme. Earlier this month, the group made its first overseas delivery, when 1.2m doses of CoronaVac were shipped to Jakarta.
Russia’s Gamaleya Institute has claimed a high level of effectiveness for its vaccine, although it has yet to complete phase 3 trials. Hannah Kuchler, Sarah Neville and Christian Shepherd
Comments